Published :
Updated :

Physicians see themselves as professionals and as healers, assisting their patients with their healthcare needs. When economists are patients, they probably see physicians the same way, but when they view doctors through the lens of economics as a discipline, they see physicians and their patients as well as economic agents. In other words, economists are interested in the degree to which physicians and patients respond to various incentives in deciding on how to deploy the resources over which they exercise their choice. Examples of issues that would concern an economist include how much time physicians devote to seeing a patient; which tests they order; what drugs, if any, they prescribe; whether they recommend a procedure; whether they refer a patient; and whether they admit a patient to the hospital. In addition, patients consider the cost when they make a decision about whether to seek care.
To say that economists view physicians and patients as economic agents is not to say that economists consider financial incentives the predominant factor in the decisions that either physicians or patients make about treatment; it is to say only that these incentives have some influence on these decisions. In fact, the role played by financial incentives in medical decision-making may often be dwarfed by the roles played by scientific knowledge, by professional norms and ethics, and by the influence of peers. However, economic policy greatly influences financial incentives, and economists tend to focus on this domain.
Physicians in all societies live and function in economic markets, although those markets vary greatly both from the simple competitive markets depicted in introductory economics textbooks and from country to country, depending on national institutions.
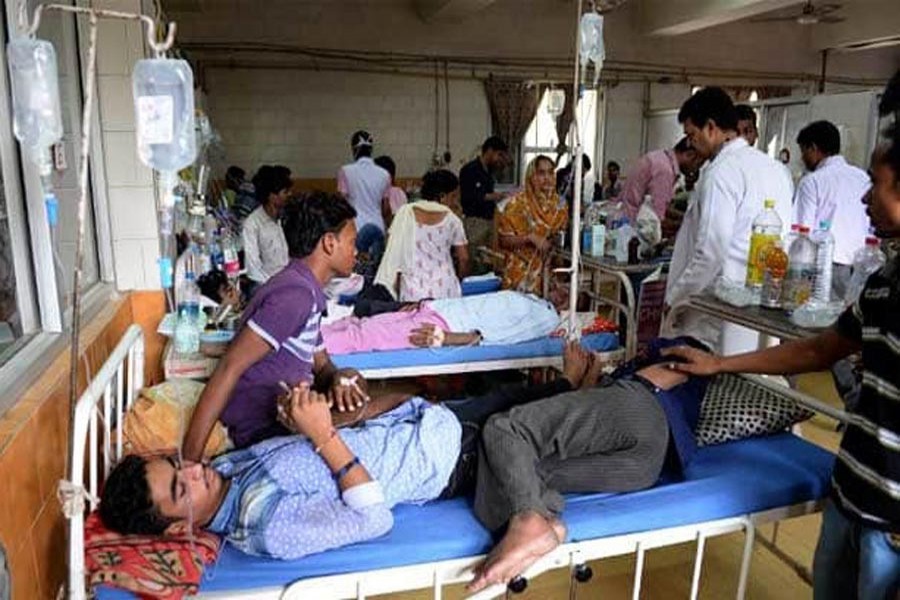
Bangladesh is a country that has seen remarkable health improvements since gaining independence in 1971, and has evolved from being a basket case to an example of good health at low cost. Although initially cautious about rallying around the goal of universal health coverage (UHC), its 2012-22 Health Care Financing Strategy provides an initial roadmap that recognises the complexities of universal coverage in a largely informal economy with a pluralistic health system and limited fiscal space. Situating their modeling exercise in this context, Rahman and colleagues extracted available UHC indicators from 17 nationally representative (in terms of epidemiology and health systems) surveys from Bangladesh. They projected that the goal of 80 per cent coverage would not be achieved for eight of 13 prevention indicators by 2030 under ceteris paribus conditions. The next 15 years, however, are likely to be characterised by rapid socioeconomic, climatic, and geopolitical forces of disruption and innovation that challenge ceteris paribus assumptions. For example, the forces of urbanisation and the growing number of urban poor who rely primarily on the private sector for care might be a massive oversight in the assessment of both service coverage and financial protection. That said, predictive modeling of this nature, with the caveats clearly spelled out, can serve as a wakeup call to policy makers in Bangladesh who might otherwise be complacent.
With respect to the projected failure to reach the target of 100 per cent financial protection, a lot needs to be done, especially in view of the latest Bangladesh National Health Accounts 1997-2015, which show an increase in the proportion of total expenditure accounted for by out-of-pocket payments from 63 per cent in 2012 to 67 per cent in 2015-pushing 4-5 million people per year into poverty. If these projections are correct, the path towards UHC is far from guaranteed, and simply staying the course will not suffice. Awareness and consensus-building at the policy and practitioner level, on the scope, contents and priorities for UHC reforms, especially with respect to the role of government, are laudable initial efforts. However, serious omissions include the absence of meaningful engagement of the rapidly growing private sector and the role of other sectors for health such as urban development, transportation, and water, sanitation, and hygiene. Furthermore, attention to the systems ingredients for better supply of services, including performance measures, health workforce development, and procurement of supplies, is sorely lacking. With respect to financing, increased efforts need to be focused on the design, implementation, and scale-up of prepayment and pooling of resources for health that will provide the opportunity for rational allocation decisions and greater efficiency, transparency, and accountability in resource use by managing the provider-purchaser split. Importantly, neither a fully government-financed nor a fully employer-financed UHC model is realistic. Rather, Bangladesh should look to similar contexts of high informality and low government financing to develop its own path forward. Implementation and operations research will also provide the relevant evidence for policy makers.
The writer is a professor of Physical Medicine and Rehabilitation at Bangabandhu Sheikh Mujib Medical University.
shahidurpmrbd@gmail.com


 For all latest news, follow The Financial Express Google News channel.
For all latest news, follow The Financial Express Google News channel.