Why Bangladesh needs an AI-driven primary healthcare revolution
Published :
Updated :

Bangladesh's healthcare system has achieved notable success over the decades, particularly in immunization, maternal health, and infectious disease control. These accomplishments are widely recognized both nationally and internationally. Yet, despite this progress, foundational weakness continues to undermine our health outcomes: the persistent neglect of preventive and primaryhealthcare. Hospitals across the country remain overcrowded, and patients largely depend on secondary and tertiary facilities even for minor health concerns. This growing pressure is not the result of individual behavior, but a reflection of systemic gaps in awareness, accessibility, and trust in community-based care.
In Bangladesh, preventive healthcare is still not part of everyday life for most citizens. Routine screening, early risk assessment, and health education and awareness are often overlooked until illness becomes severe. Many people do not priorities preventive services, and spending money on healthcare is frequently seen as necessary only when disease strikes. This mindset leads to delayed treatment, increased complications, and rising healthcare costs for families. It also places an unsustainable burden on hospitals that should primarily be serving patients requiring specialized care.
The consequences of weak primary healthcare are becoming even more serious as Bangladesh faces a rapid rise in non-communicable diseases such as diabetes, hypertension, obesity, and mental health disorders. These conditions are no longer confined to older populations; they are increasingly affecting working-age citizens and threatening the nation's productivity. Bangladesh has a large youth population and the potential to benefit greatly from a demographic dividend, but that opportunity is at risk if chronic illnesses continue to spread without early detection and preventive intervention.
Urbanization has further complicated the situation. In urban areas, primary healthcare services remain fragmented, uncoordinated, and insufficient. As a result, people depend heavily on large hospitals even for basic health needs. Rural communities, meanwhile, continue to experience limited access to integrated and quality preventive and primary healthcare. Strengthening primary healthcare across both rural and urban areas is therefore no longer optional; it is essential for national health security.
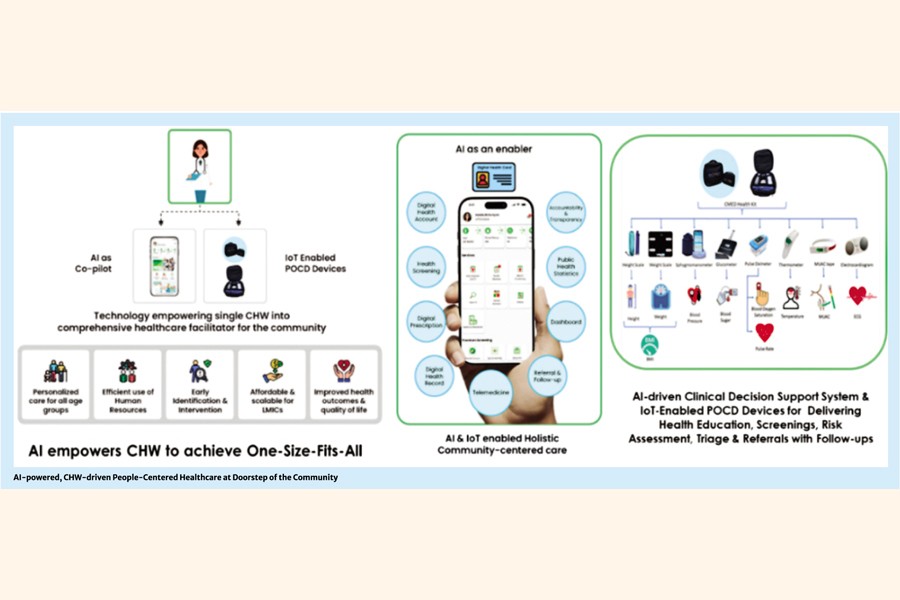
In response to these pressing challenges, United International University (UIU) and CMED Health have jointly developed Intelligent General Practitioner (iGP) Model, an innovative approach designed to bring preventive and primary healthcare directly to people's doorsteps. iGP model is an Artificial Intelligence (AI) powered, Community Health Workers (CHWs) anchored human-centered model with an integrated GP Center in the community designed to deliver comprehensive preventive and primary healthcare including referral and follow-up at people's doorsteps for enhancing well-being, productivity & happiness.
iGP model creates a digital health account for every citizen and ensures periodic health education, check-up for early identification & timely intervention of health issues, transforming sick-care into proactive, promotive and preventive care for reducing catastrophic health expenditure to alleviate poverty. CHWs, empowered & equipped with AI-driven clinical decision support system with Internet of Things (IoT) based Point of Care Diagnostic (POCD) devices, visit households in the communities to deliver health education, conduct periodic screenings, risk assessment, triage and provide referrals with follow-ups. This ensures every family member (new born, children, adolescents, adult, pregnant women & elderly) receives personalized preventive and primary healthcare with proactive management. This innovative AI-powered approach ensures one CHWs addressing diverse health needs of every household in the community and empowering them as well as mitigate acute shortage of providers. When necessary, patients are connected to 24/7 audio or video telecomsultation services for immediate management of health concerns. The model also integrates a physical clinic within the community staffed with General Practitioner (GP), Nurse, Paramedic, Midwives and other support staffs with necessary medical equipment to deliver comprehensive primary healthcare aligned with Essential Service Package (ESP) and emphasis on NCDs, Maternal Health Services and Normal Deliveries. The physical clinic ensures quality GP consultations (~10 Minutes) with empathy and other preventive and primary care services. This AI-integrated solution able to manage up-to 90% of health issues within the catchment area (Union/Ward). When higher-level care is required, iGP facilitates timely referrals and connects users to the right resources at secondary/tertiary facilities with in the hospital networks.
Drawing inspiration from Bangladesh's successful community-based initiatives like family planning and immunization, iGP leverages 4IR technologies to address fragmentation in the health system. It includes clinically validated screening tools for Autism, Breast Cancer, Dementia & Alzheimer's Disease, Parkinson's Disease, and Eye Care-bringing early detection and intervention to populations that are often left behind. By capturing and analyzing individual and household/population-level health data, iGP supports data-driven decision-making, enables predictive analytics for public health planning, and lays the groundwork for establishing AI-powered social health protection in resource-constrained settings. The model's end-to-end accountability, enabled by real-time, trackable data, ensures greater systemic efficiency. Mirroring Bangladesh's success in mobile and financial inclusion, iGP promotes "Health Inclusion" (2021-2030), making it not only a scalable and adaptable model for UHC but also a game-changing innovation for low-resource settings worldwide.
Over the past 10 years, iGP has impacted 3+ million lives through the creation of digital health accounts and providing people-centered comprehensive preventive and primary healthcare solution by working directly with community health workers, serving both rural & urban populace, employees & factory workers, adolescents, adults, women & aging population to understand their pain points and tailor solutions accordingly. The earlier version of iGP named as Digital General Practitioner Model, has been successfully implemented in Bangladesh. In partnership with local NGOs, the integrated platform has scaled & served over 2.5+ million individuals from 450,000+ families across 65 catchment areas, empowered 3000+ female health workers achieving 99.5% service satisfaction rate. Recognizing different urban healthcare challenges, model was adapted the for urban communities. Under the management of UNICEF and partnership with PHD & Nari Maitree, and funding from the Swedish International Development Cooperation Agency (SIDA) iGP Model named as "Aalo Clinic" is implemented in 6 locations at Karail, Mirpur, Shyampur, Dhalpur, Ershad Nagar, and Narayanganj where 580,000+ patients have been served so far. The updated version of iGP model branded as "Amader Susastho" located at Uttara, Dhaka, offering a seamless, tech driven urban primary healthcare through an integrated service delivery framework to provide accessible, and affordable quality healthcare for individual and family. iGP model offers services just at $1/rural family and $3/urban family towards ensuring long?term viability.
Bangladesh's Health Reform Commission has already emphasized primary healthcare as a constitutional right and recommended free access alongside digital health accounts for every citizen. iGP model aligns strongly with this vision and offers a pathway toward Universal Health Coverage (UHC). By integrating AI, community outreach, and digital health infrastructure, Bangladesh has an opportunity to build a strong, people-centered healthcare system that reduces poverty, improves productivity, and ensures health security for all. iGP model is also aligned with the visionary "Three Zero Theory"-zero poverty, zero unemployment, and zero carbon emissions. By ensuring affordable and quality healthcare, the model helps identify health risks and detect diseases early, reducing catastrophic health expenditure and poverty. If implemented widely, household-based data collection will allow identification of each family member and enable targeted interventions in education, skills development, and employment to reduce unemployment.
Future governments can effectively utilize iGP model to ensure accessible preventive and primary healthcare at the community level and build a strong, people-centered health system through health education, regular screening, NCD management, and digital health integration. This will reduce health risks and costs, keep the workforce healthy, and accelerate national development. We believe healthcare should not begin only after illness occurs-preventive care before disease is the best approach. iGP model works toward ensuring that by 2030 everyone is covered under primary healthcare, and no one falls into poverty due to health expenses. According to statistics, nearly one-fourth of Bangladesh's population consists of youth, close to 50 million people. These young individuals can become future innovators, leaders, and drivers of social change. iGP model encourages youth engagement in health awareness, leadership, and community service. We must move beyond the mindset of "treatment after disease" and invest in prevention, early detection, and community-based healthcare delivery. iGP model offers a timely, proven, and sustainable solution.
Khondaker A. Mamun, PhD. is Professor, Artificial Intelligence (AI) Director, IRIIC, United International University and founder, AI Forum Bangladesh


 For all latest news, follow The Financial Express Google News channel.
For all latest news, follow The Financial Express Google News channel.