Benefits and costs of social distancing in rich and poor countries
Zachary Barnett-Howell, Oliver John Watson and Ahmed Mushfiq Mobarak
Published :
Updated :

With circumstances previously not thought of, the Covid-19 pandemic has given rise to a series of heated debates regarding which public health measure would be most effective to contain the virus in absence of a vaccine. Many governments around the world implemented social distancing and lockdown measures intending to minimise transmission within a certain time by allowing targeted testing and tracking protocols. Alongside containment measures, an important discussion has arisen on the economic repercussions of lockdowns and suppression, particularly in countries with low per capita income. Keeping those countries in mind, it is a question worth asking whether shutting down the economy for months was a reasonable burden to carry. In higher-income countries, like the United States, proper benefit-cost metrics suggest that aggressive suppression measures and social distancing practices are logical for the economic welfare of their population.
The study titled "The Benefits and Costs of Social Distancing in Rich and Poor" analyses the differing Covid-19 suppression strategies in low and middle-income countries by putting a value on said strategies. It is projected that Covid-19 mortality sharply increases with age, and lower-income countries have a relatively younger population. It can be, thus, assumed that lower-income countries face a lower mortality risk from the virus. But these countries are, however, unable to cope with the rapidly growing Covid-19 cases with their unequipped healthcare system. This indicates the improbability to contain the spread of the virus without any significant mitigation effort in lower-income countries.
The populations in the low-income countries are less willing to trade off their economic livelihood with lockdown measures, which implies that the economic welfare value of reducing Covid-19 mortality risk may be lower in those countries as well. The poorest of the population in these countries live overwhelmingly close to the subsistence levels. Without proper social protection and safety nets in place, the burden of social distancing through lockdown, which for them is economic distancing too, may push a huge portion to immediate deprivation and hunger. In this scenario, poorer households may not be able to comply with lockdown measures due to their strong reluctance to trade their livelihoods with "probable" risk reduction. In countries that have a relatively weaker enforcement capacity, the situation may worsen in two aspects: a collapse in the formal economy, and a continued spread of the virus led by the continuation of the informal economy.
To compare the relative value of suppression in rich countries with that of the poor countries, the study integrates the country-specific cost estimates with the epidemiological model, which projects cross-country mortality from the spread of Covid-19, developed by the Imperial College London. Two researchers [Greenstone and Nigam (2020)] predict that social distancing measures could save 1.76 million lives in the United States, directly and indirectly by reducing hospital overcrowding, with a total welfare value of 7.9 trillion USD.
The age-structured compartmental SEEIR model designed by the Imperial College London takes the demography and healthcare capacity of each country into account and simulates the hospitalisation and fatality caused by Covid-19. The model assigns an age-specific mortality probability to individuals who receive health care and a higher mortality likelihood to individuals who need but cannot receive hospital care due to inadequate capacity. The study holds a base estimated infectivity (R0) for Covid-19 for each country and estimates mortality rates under five different scenarios where the infectivity of the virus has been modified to represent the implementation of a social distancing policy in each country. In each of the scenarios, the policy remains in effect for a period of forty days, the average duration of most lockdown and social distancing policies around the world.
The study includes 178 countries which are classified as high, upper-middle, lower-middle, and low-income economies by the World Bank Country and Lending Groups 2020. Data on life expectancy for each age group are extracted from the World Health Organisation Global Health Observatory.
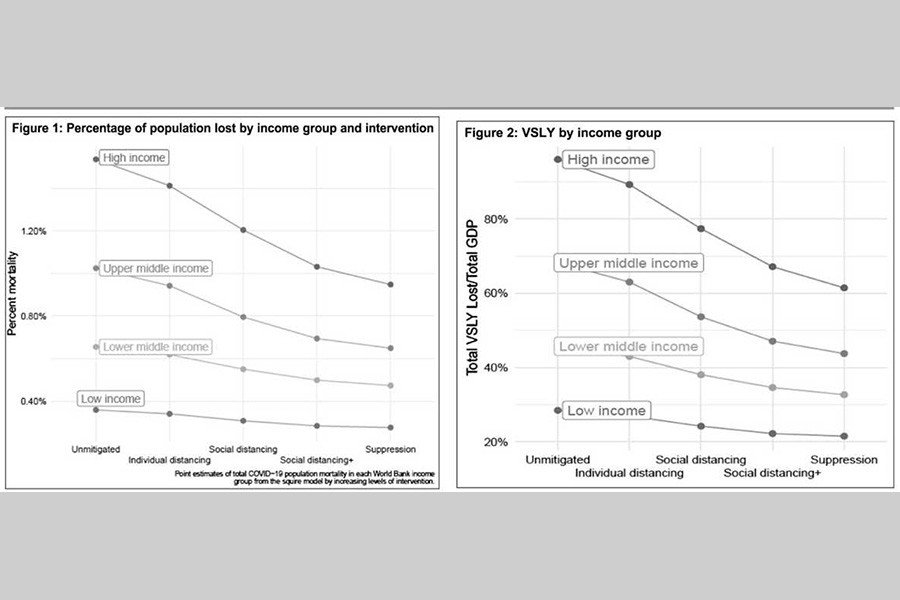
The model predicts that for richer countries like the United Kingdom and the United States, the unmitigated spread of Covid-19 could lead to more than 1.2 per cent deaths. On the other hand, in poorer countries like Nigeria, Pakistan, and Bangladesh predicted mortality is approximately half that. In the United States and the United Kingdom, mortality falls sharply after imposing social distancing measures. But the change in mortality in lower-income countries is significantly unresponsive to a greater extent when social distancing measures are imposed. Aggregating the total predicted mortality under each scenario by total population across all four income groups, the study finds that expected mortality is lower in poorer countries despite their uncapacitated healthcare systems.
Age-specific mortality parameter estimates that the proportion of cases that require hospitalisation increases with age, up to nearly 20 per cent of the elderly, who are aged 75 and above. The analysis finds that the mortality rate is low for those under the age of 60, covering nearly 60 per cent of the elderly, for patients hospitalised but not requiring critical care. The likelihood of death doubles, up to a maximum of 90 per cent, for patients who require but don't receive hospital care due to constrained capacity (Verity et al. 2020; Walker, Watson, et al. 2020). As the population in lower-income countries is heavily skewed younger, a much smaller fraction of their population is predicted to be hospitalised for or die from Covid-19.
To determine the relative value of social distancing and lockdown measures, the study incorporates country-specific estimates of the welfare value of risk reduction, the value of a statistical life (VSL) and the value of a statistical life-year (VSLY), with the mortality predictions. VSL, a metric of the economic value of risk, is used to provide a valuation for the likelihood of mortality that can be reduced. VSL suggests that imposing and implementing social distancing measures yield a significant welfare improvement in richer countries, but a declining value in poorer countries.
With no mitigation effort in place, Covid-19 has a large relative welfare cost in high-income countries-approximately 250 per cent of the GDP of the United States. On the contrary, unmitigated situations see losses approximately half that in India, Bangladesh, Pakistan, Nigeria, Nepal when scaled against their respective GDP. A full-fledged social distancing policy for a 40-day period that decreases the infectivity of Covid-19 to 35 per cent of its base value is estimated to yield a welfare value equal to 64.6 per cent of the UK's annual GDP and to 53.4 per cent of that of the United States. The same policy stance in India yields a welfare increase equivalent to only 14.6 per cent of its GDP and in Bangladesh only 13.1 per cent of its GDP.
The VSLY, used in assigning value to mortality risk reduction when the benefits are spread across a population, is derived by dividing the country-specific population-averaged VSL by the life expectancy of a working-age person, someone between the ages of 20-64. The use of the VSLY instead of the VSL supports the conclusion of the study that the value of social distancing and other measures to contain Covid-19 is unequally distributed between rich and poor countries. Estimates show that social distancing provides a welfare value of more than 30 per cent of GDP in countries like the UK and the US, whereas an identical policy generates a welfare gain of less than 10 per cent in lower-middle and low-income countries.
The economic opportunity cost of social distancing is much greater in poorer countries, and thus the VSL is lower. In simpler words, wealthy people can meet their basic needs more easily in social distancing, while a poor person is forced to choose income-generating activities to provide for their family. Workers in poorer countries are more likely to rely on a daily cash wage and as their work is mostly hands-on, they cannot maintain distance while working. Even if a social insurance policy were implemented in these countries, there remain uncertainties regarding how quickly such people could be located, if at all, to deliver relief benefits to them. Moreover, cross-country results find that a 1.0 per cent decrease in GDP can lead to an increase in infant mortality between 0.24 and 0.40 per 1,000 children born.
The study urges for a policy whose benefits are weighed carefully against the economic costs and risks imposed on a society. Although it is certain that the risks that economic shutdowns pose on the most vulnerable members of low-income societies, it is yet to be determined whether the value of the strict suppression policies in poor countries outweighs the uncertain economic costs. A full-fledged assessment is crucial to ascertain other measures that could effectively preserve lives and aggregate welfare. Harm-reduction measures, such as increasing access to clean water and handwashing facilities, universal mask-wearing, targeted social isolation of the at-risk groups, providing food, fuel and cash to people at risk of hunger and deprivation during lockdowns, may allow the people in the low-income countries to minimise Covid-19 risk while maintaining the ability to put food on their tables.
[This article provides a summary of the key findings of the paper titled "The Benefits and Costs of Social Distancing in Rich and Poor Countries" published in the journal "Transactions of the Royal Society of Tropical Medicine and Hygiene"]
Zachary Barnett-Howell is a Postdoctoral Associate at Yale University. zachary.barnett-howell@yale.edu
Oliver John Watson is affiliated with the MRC Centre for Global Infectious Disease Analysis, Department of Infectious Disease Epidemiology, Imperial College London, London, UK
Ahmed Mushfiq Mobarak is a Professor of Economics at Yale University. ahmed.mobarak@yale.edu


 For all latest news, follow The Financial Express Google News channel.
For all latest news, follow The Financial Express Google News channel.